Health
Anyone confronted with climate events can directly or indirectly experience impacts on their physical and mental health. The damage can vary depending on the individual’s health determinants. It may be worse if the person’s living environment, state of health or socio-economic situation are already fragile.
Damage to physical health
Indirect physical damage through impacts on living environments
The effects of climate change may appear in the form of personal injury as a result of a chain of impacts. Rising temperatures (a direct impact of climate change) can contribute to summer droughts (a direct consequence of this impact), making forests more fragile. This makes them more vulnerable to the spread of forest fires. This was the case in the village of Lytton, British Columbia, which went up in flames in July 2021. In an event of this kind, damage to buildings, infrastructure and trees can cause objects and debris to fall. The population may then suffer physical injuries indirectly linked to climate change.
Other hazards that are expected to worsen with climate change, such as floods and landslides, storms with strong winds occurring in any season, and even freezing rain events, can deteriorate the living environment, cause widespread destruction and thus be indirectly responsible for personal injury.
Direct bodily harm through impacts on general health
Bodily injury can occur when an individual is directly injured by the climate event. For example, during freeze-thaw or freezing rain events, road surfaces may be covered with ice, leading to falls and injuries.
The climate event can also affect an individual’s internal system. The body can activate physiological mechanisms to protect itself, creating a cascade effect of unwanted symptoms. This can be the case, for example, during a heatwave, which can cause heatstroke, dizziness, dehydration, physical fatigue upon exertion, increased heart rate and even cardiac arrest. The living environment can also act as a heat amplifier. This is particularly true if surrounding hard surfaces (made with asphalt, concrete and tar) are numerous and dark in colour, as they absorb heat during the day and re-emit it at night. As a result, outdoor workers are highly exposed to heatstroke, and even more so when their activities take place near this type of surface.
Certain climate events can also affect respiratory capacity (asthma) or increase allergic symptoms (nasal secretions and eye irritation). This is particularly true of rising concentrations of fine particles and ozone in the air, as well as forest fires, which are responsible for smoke poisoning. The same is true of summer storms, which trigger the production and release of allergens into the air. When rain events are combined with strong winds, this facilitates the detachment and dispersal of pollen.
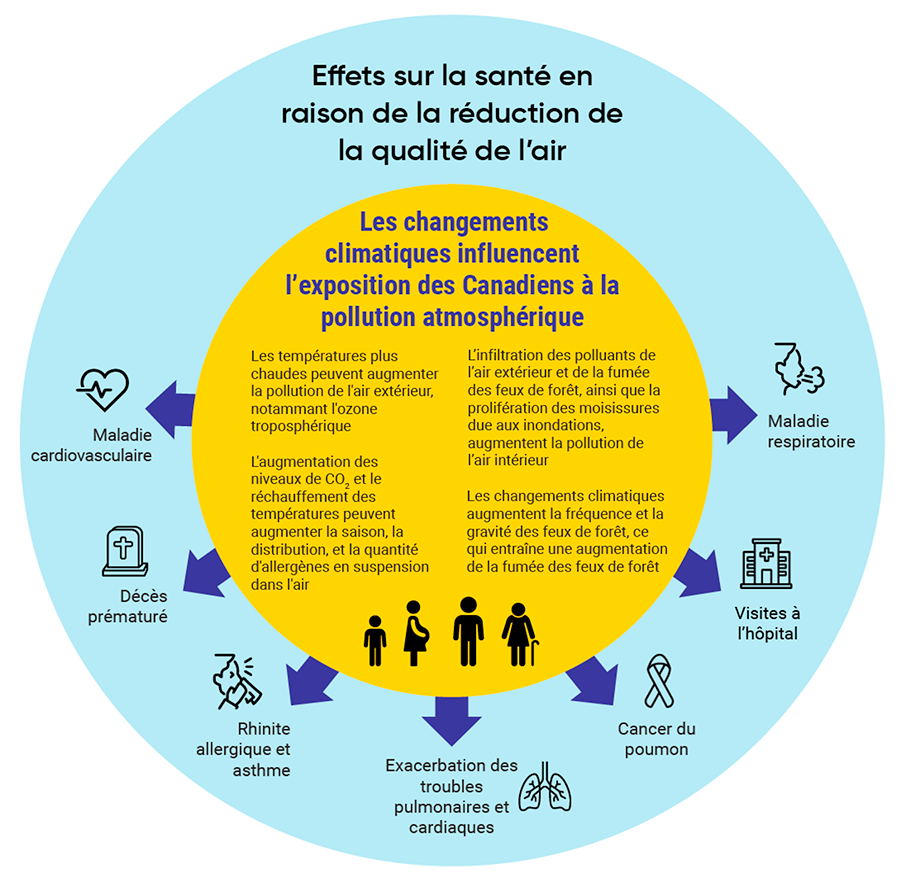
Figure 1: Health effects due to reduced air quality.(source : Berry, P., et Schnitter, R. (éd.). (2022). La santé des Canadiens et des Canadiennes dans un climat en changement : faire progresser nos connaissances pour agir. Ottawa (Ontario) : government of Canada.
Climate change is also responsible for deteriorating water quality (see the page on Water Availability and Quality), which in some contexts can affect people’s physical health. The presence of certain bacteria in water, such as Campylobacter and Escherichia coli, is favoured by warmer temperatures and low water flow. These bacteria can cause diarrhea, dehydration and, in extreme cases, death.
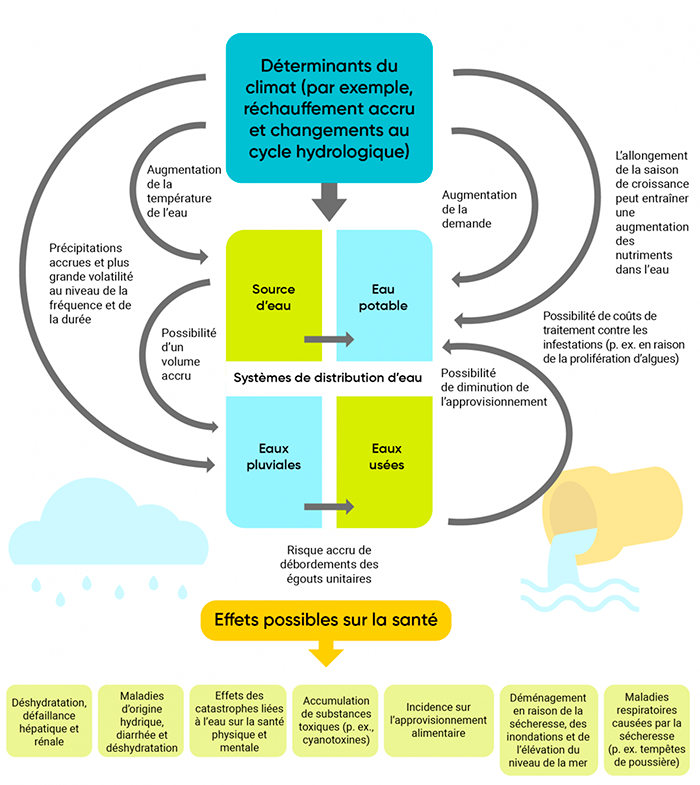
Figure 2 : Impacts of climate change on water quality and quantity, and repercussions on health.(Source: Berry, P., et Schnitter, R. (éd.). (2022). La santé des Canadiens et des Canadiennes dans un climat en changement : faire progresser nos connaissances pour agir. Ottawa (Ontario) : government of Canada.
Visit our Ecosystems page to learn more about the spread of harmful species.
Due to the earlier arrival of spring and the later arrival of autumn in Quebec, vegetation has a longer growth season. The means that pollen production and the allergy season lengthen. The allergy season is divided into three periods:
-
March to June: tree and shrub pollen
-
May to October: pollen from grasses and hay
-
July to October: ragweed pollen
What’s more, Quebec’s warmer summers and winters are increasingly favourable to the spread of pest species that migrate north. Among them, several are likely to carry diseases (see the Ecosystem section). This is true of several insects that can transmit diseases to humans, such as West Nile virus, Lyme disease and even moulds, which multiply in humid environments.
Bodily harm by means of impacts on the determinants of health inequity
Health inequity factors can compromise people’s ability to make the right choices when it comes to treating themselves or protecting themselves from extreme weather events. For example, a person with a low income does not have the financial capacity to adapt their home to hot weather if it is poorly insulated and ventilated. During a heatwave, the heat accumulated over several days and nights inside the home can lead to a deterioration in the individual’s physical condition, potentially resulting in hospitalization (see the Urban Environment page).
Damage to mental health
Climate hazards can cause damage to an individual’s mental health, either through the emotional load that increases at the time of the event, or through the development of post-traumatic shock.
Situations arising after the extreme event can also be difficult to handle. Dealing with the repair of damage, the rebuilding of personal property and housing, and the loss of loved ones can all be very stressful for an individual. In 2011, the Climate Institute demonstrated that the psychological consequences of a climate event can persist for months or even years, affecting individuals and entire families.
Furthermore, the continuous, frequent, violent and increasingly visible impacts of climate change are generating ecoanxiety. People’s fear for the fate of the planet and their sense of powerlessness in the face of current environmental challenges are increasing the incidence of depression. A study conducted at the Université de Sherbrooke in 2021 showed that almost half (49%) of young adults (ages 18-24) surveyed had experienced at least one manifestation of ecoanxiety in the two weeks preceding the survey, compared with 26% of the general population.
Health services
During an extreme event, the emergency situation and the ensuing surge in demand put pressure on healthcare services in terms of hospital staff, emergency or inpatient wards, ambulance transport, and more. From an infrastructure point of view, many healthcare facilities were not built to withstand certain climate events, such as high winds, excessive indoor temperatures or flooding.
Their critical systems (medical equipment in operating theatres and intensive care units, etc.) or the buildings themselves (roofing, cladding, windows, pipes, electrical system) could therefore be damaged, which could disrupt the provision of care. From an individual point of view, healthcare staff could also be affected by a climate event and miss work if roads are impassable, for example, or if they themselves are affected by the event.
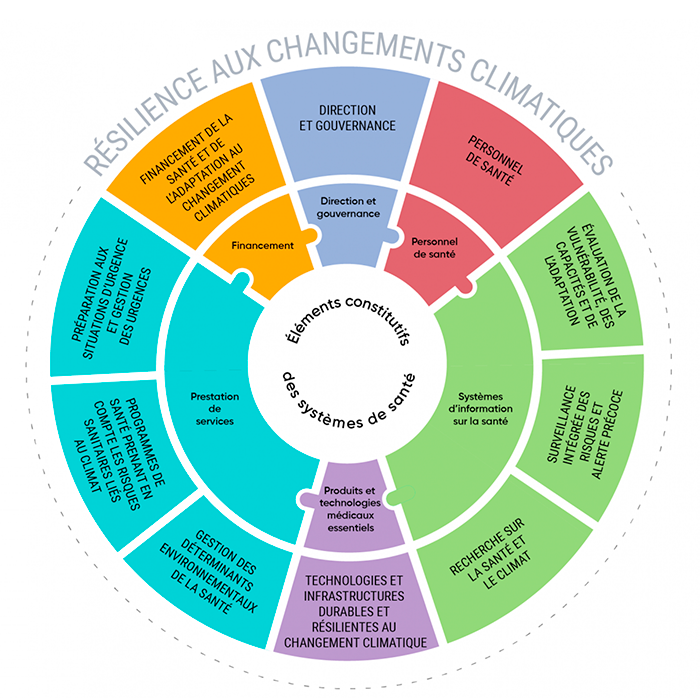
Figure 3 : Ten elements of the WHO’s operational framework for building climate resilient health systems. (Source: Berry, P., et Schnitter, R. (éd.). (2022). La santé des Canadiens et des Canadiennes dans un climat en changement : faire progresser nos connaissances pour agir. Ottawa (Ontario) : government of Canada.)
Last update of the page : December 2022.